Summary:
Telehealth apps are reshaping how healthcare is delivered by making consultations, monitoring, and follow-ups more accessible and efficient. This guide covers essential features, benefits for providers and patients, and how AI reduces manual work. It also highlights the role of a reliable Telehealth App Development Company, along with the development process, cost factors, challenges, and future trends shaping modern, scalable, and patient-focused healthcare systems.
Healthcare is changing quickly, but not in a flashy way. It’s more of a steady shift that people working in the system can clearly notice.
Patients don’t want to wait weeks just to see a doctor. At the same time, healthcare providers are dealing with too much paperwork and packed schedules. It’s becoming harder for both sides to keep up. Because of this, there’s a growing need to make healthcare simpler and easier to access.
That’s where Telehealth App Development comes in. It’s not just a trend, it’s a practical way to help doctors and patients connect more easily and manage care better. Let’s get into it properly.
Why Telehealth Is Becoming a Core Part of Modern Healthcare
A few years back, telehealth felt like a backup plan. Now it’s becoming a default option in many cases.
Rising demand for remote care and convenience
People are used to doing everything from their phones banking, shopping, even therapy sessions. So, expecting them to travel for every consultation feels a bit outdated. Telehealth removes that friction.
Shift in patient expectations toward digital-first experiences
Patients today don’t just compare healthcare providers they compare experiences. If one clinic offers smooth online booking and instant consultations while another requires calls and waiting the choice is obvious.
Pressure on providers to improve access and efficiency
Hospitals and clinics are dealing with higher patient volumes than ever. Telehealth helps manage that load by handling non-critical consultations remotely, freeing up physical space for urgent care.
Role of AI automation in reducing manual workload
This part’s honestly a game changer. AI tools can manage scheduling, collect patient data, and even assist in documentation. It doesn’t replace human judgment, it just removes repetitive work that slows everything down.
How telehealth fits into long-term healthcare delivery models
We’re moving toward hybrid care. Some visits happen in person, others online. It’s not about replacing traditional care, it’s about making it more flexible and accessible.
Telehealth App Development: Understanding the Bigger Picture
When most people hear telehealth, they picture a video consultation. That’s just the surface. Healthcare App Development today is about building complete digital ecosystems that support the entire care journey.
What telehealth apps actually include beyond video calls
Think scheduling systems, patient records, billing, messaging, analytics, everything connected in one place.
Key stakeholders: patients, doctors, admins, care teams
It’s not just doctor and patient anymore. Nurses, coordinators, and admin staff all interact with the system. So the app has to work for everyone, not just one group.
Difference between basic telemedicine and advanced digital care platforms
Basic telemedicine = consultation.
Advanced platforms = continuous care, monitoring, data insights, follow-ups the whole journey.
Where AI automation enhances decision-making and workflows
AI can flag high-risk patients, suggest next steps, and even prioritize cases. It’s not replacing doctors, it’s helping them move faster and smarter.
Core Features Every Telehealth Platform Should Include

If you’re building a telehealth platform, these features aren’t optional, they’re foundational.
- Secure video consultations and real-time chat: This is the core experience. Video calls should be stable, clear, and secure. Even small lags or glitches can frustrate users.
- Appointment scheduling and automated reminders: Manual scheduling is messy. Automated systems reduce missed appointments and help providers manage time better.
- EHR/EMR integration for seamless data access: Doctors need context. Without access to patient history, even simple consultations become inefficient.
- E-prescriptions and digital payments: Patients shouldn’t have to switch between systems. Everything from consultation to payment should happen in one smooth flow.
- AI-powered symptom checking and triage support: Before even meeting a doctor, patients can input symptoms. This helps prioritize cases and saves time during consultations.
- Patient dashboards and doctor panels: Dashboards keep everything organized: appointments, reports, prescriptions. Doctors and patients both need clear visibility.
Benefits for Providers and Patients
Telehealth isn’t just about convenience, it improves how healthcare works on both sides.
- Improved access to care: Patients in remote areas or with mobility issues can get medical help without traveling long distances.
- Reduced operational burden: Less paperwork, fewer physical visits, and better scheduling systems make operations smoother.
- Better patient engagement: When care is easier to access, patients are more likely to follow up, attend appointments, and stay involved.
- Cost efficiency: Providers save on infrastructure costs, while patients save on travel and time.
- Faster decision-making with AI support: AI tools help doctors process information quickly, leading to faster and often more accurate decisions.
How AI Automation Is Transforming Telehealth App Solutions
AI isn’t just an add-on anymore, it’s becoming a core part of Telehealth app solutions.
Smart appointment scheduling and no-show reduction
AI can analyze patterns and suggest optimal appointment slots. It can even predict when patients might miss appointments.
AI chatbots for patient support and intake
Basic queries don’t need human intervention. AI Chatbots can handle FAQs, onboarding, and initial data collection instantly.
Clinical decision support systems
AI can assist doctors by analyzing patient data and suggesting possible diagnoses or treatments. It’s not perfect, but it’s useful.
Automated documentation and voice-to-text notes
Doctors spend less time typing and more time interacting with patients. Conversations can be converted into structured medical notes.
Predictive analytics for patient monitoring
AI can detect early warning signs by analyzing trends in patient data. This helps in proactive care.
Personalized care recommendations
Treatment plans can be tailored based on patient behavior, history, and real-time data.
Ensuring Compliance, Security, and Data Privacy
Healthcare data is sensitive. There’s no room for mistakes here.
Importance of regulatory compliance (HIPAA, GDPR, etc.): Healthcare apps must follow strict regulations depending on the region.
Non-compliance can lead to serious consequences: Secure data storage and encryption practices: Patient data must be encrypted at all stages of storage, transmission, and access. No exceptions.
User authentication and access control: Different users need different levels of access. Role-based permissions help protect sensitive data.
Risks of non-compliance and how to avoid them: Legal issues, fines, and loss of trust all of it can happen if compliance is ignored.
Building trust with patients through transparent data handling: Patients are more likely to use digital healthcare if they trust how their data is handled.
Telehealth App Development Process: From Idea to Launch
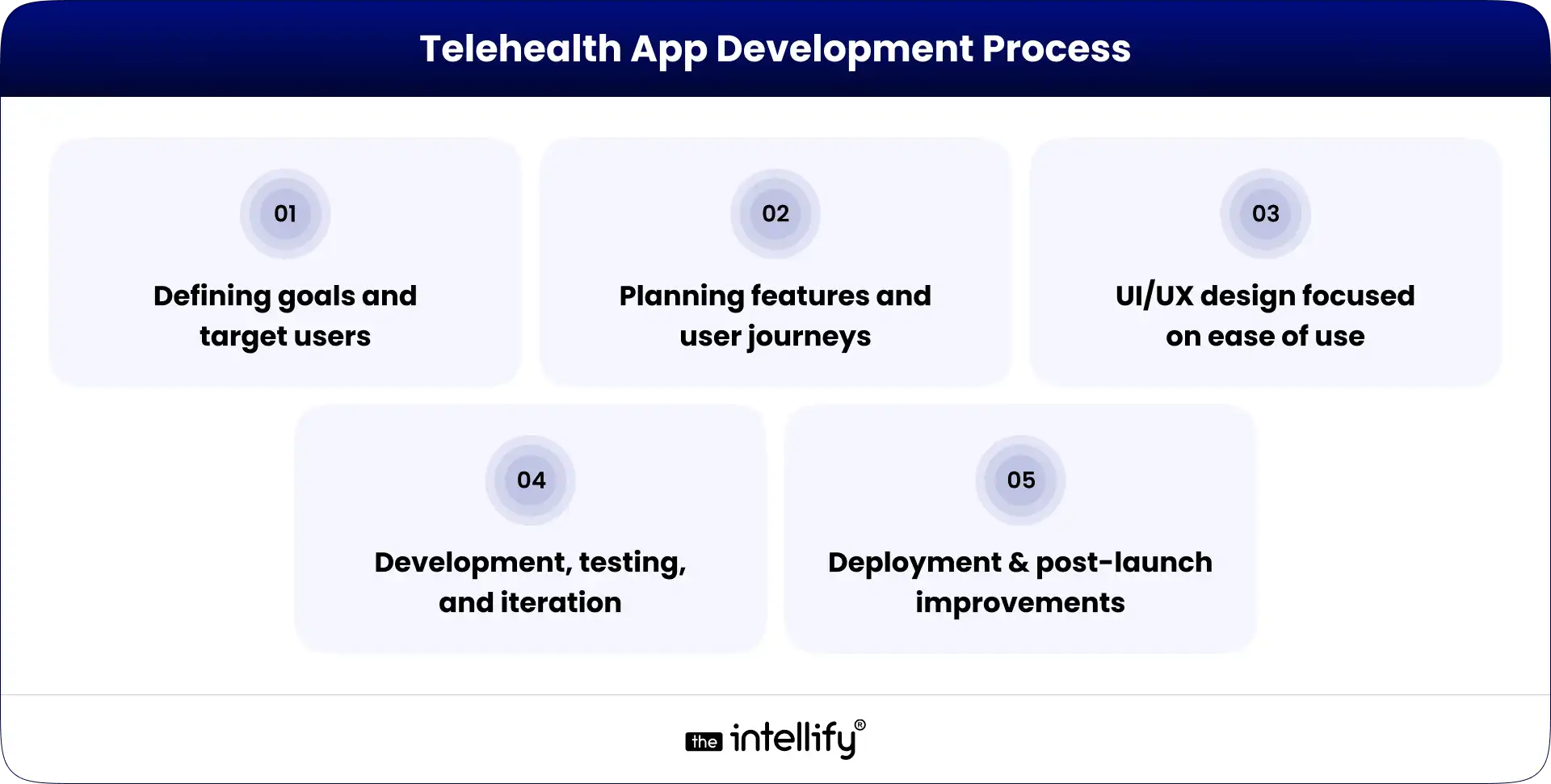
Building a telehealth app isn’t just about writing code, it’s about solving real problems step by step, with a clear plan from the start.
Defining goals and target users
Everything begins with clarity. You need to understand who the app is for patients, doctors, or both and what exact problem you’re trying to solve. Without this, it’s easy to build something that looks good but doesn’t really help anyone.
Planning features and user journeys
Once the goals are clear, the next step is mapping how users will move through the app. From booking an appointment to completing a consultation, every step should feel simple and natural. If the journey feels confusing, users will drop off.
UI/UX design focused on ease of use
Design matters more than people think. Healthcare apps are used by all age groups, so the interface needs to be clean, clear, and easy to navigate. If users have to “figure things out,” it usually means the design needs improvement.
Development, testing, and iteration
This is where the actual build happens, but it’s not a one-time process. The app is developed in phases, tested regularly, and improved based on feedback. Issues will come up that’s normal. The key is fixing them early.
Deployment and post-launch improvements
Launching the app isn’t the end, it’s just the beginning. Real users will interact with it in unexpected ways, and their feedback helps shape future updates. Continuous improvements are what keep the app relevant and useful over time.
Cost Factors That Influence Telehealth App
Costs can vary a lot. And yeah, it depends on what you’re building.
- Feature complexity and customization level: More advanced features increase development time and cost.
- Integration requirements (EHR, payment systems, etc.): Connecting with existing systems adds layers of complexity.
- AI capabilities and data infrastructure: AI requires data, processing power, and continuous tuning.
- Development team structure and location: Costs differ based on whether you’re working with in-house teams or external partners.
- Ongoing maintenance and updates: Apps need regular updates, security patches, and improvements.
Common Challenges in Building Telehealth Platforms
It’s not all smooth. Some challenges are kinda unavoidable.
- Integration with legacy healthcare systems: Older systems aren’t built for modern integrations. APIs and middleware help bridge the gap.
- Managing data security at scale: As your user base grows, so do security risks. Planning early helps avoid bigger issues later.
- Ensuring a smooth user experience for all age groups: Not everyone is comfortable with technology. Simplicity matters more than design trends.
- Handling real-time communication without lag: Video and chat systems need a strong infrastructure. Even slight delays can affect user experience.
- Balancing innovation with compliance requirements: You can’t move fast and break things in healthcare. Everything needs to be controlled and compliant.
Real-World Use Cases Across Healthcare Segments
Telehealth is already being used across different areas, and it’s only expanding as providers find more practical ways to apply it.
Virtual consultations for general practice
Patients can handle routine check-ups, minor illnesses, and follow-ups without visiting a clinic. It saves time for both patients and doctors, especially for non-urgent cases.
Remote patient monitoring for chronic conditions
For conditions like diabetes or hypertension, continuous monitoring helps doctors track progress without frequent in-person visits. It also allows early intervention if something seems off.
Mental health and therapy platforms
Online therapy has made mental health support easier to access. Patients often feel more comfortable attending sessions from home, which improves consistency.
Post-surgery follow-ups and rehabilitation
Recovery doesn’t always require hospital visits. Patients can share updates, attend follow-ups, and receive guidance remotely while recovering at home.
Rural and underserved area healthcare access
Telehealth helps bridge the gap where medical facilities are limited. Patients in remote areas can connect with specialists without long travel, improving overall access to care.
What to Look for in a Telehealth App Development Company
Choosing the right Telehealth App Development Company can make or break your project. It’s not just about technical skills, it’s about understanding healthcare, users, and long-term goals.
Experience in healthcare and compliance standards
Healthcare is complex, with strict regulations and workflows. You need a team that already understands compliance requirements like HIPAA or GDPR, not one that’s learning on the go.
Ability to integrate AI automation effectively
AI should simplify processes like scheduling, patient intake, and documentation. A good team knows where AI adds value, and where it might just create confusion.
Strong portfolio and proven case studies
Past work gives you a clear picture of what the company can deliver. Look for real projects, not just concepts, especially in healthcare or similar regulated industries.
Focus on scalability and long-term support
Your app shouldn’t feel limited after launch. It should be built to scale as your user base grows, with ongoing support for updates, security, and new features.
Clear communication and transparent processes
If communication feels unclear or slow in the early stages, that’s usually a sign of bigger issues later. You want a team that keeps things simple, honest, and easy to follow. Healthcare-focused companies like The Intellify are often involved in projects where ongoing collaboration and clarity matter throughout development.
Future Trends in Telehealth and AI-Driven Healthcare
This space is evolving quickly, and honestly, it’s not slowing down anytime soon. What we’re seeing right now is just the early version of what telehealth can actually become. A lot of things that felt “advanced” a few years ago are now becoming standard.
Expansion of AI-powered diagnostics
AI will support doctors by analyzing data faster and spotting patterns early. It won’t replace clinical decisions but will help improve accuracy and speed.
Integration with wearable devices and IoT
Health data from devices like smartwatches will connect directly with telehealth apps, giving doctors a more continuous view of patient health.
Real-time health analytics and alerts
Systems will track patient data in real time and send alerts when something seems off, helping providers act earlier.
Hyper-personalized patient experiences
Care plans will become more tailored based on individual health data, making treatment more relevant.
Growth of decentralized and home-based care models
More care will shift from hospitals to homes, supported by telehealth platforms and connected devices.
Final Thoughts
Building a telehealth app isn’t about adding more features; it’s about solving real problems. If patients struggle to book appointments or join consultations, the tech doesn’t really matter.
The key is balancing innovation with usability and trust. Healthcare apps need to feel simple and reliable, not complicated. AI automation will keep playing a role by reducing manual work and helping providers make faster decisions, but it has to be used carefully.
In the end, a well-built telehealth platform improves access, reduces effort for providers, and makes care more efficient. That’s what actually matters.
Frequently Asked Questions (FAQs)
1. How long does it usually take to build a telehealth app?
It depends on the features and complexity. A basic version can take 3-4 months, while a fully integrated platform with AI, EHR, and advanced features may take 6-9 months or more.
2. What makes a telehealth app actually successful in real use, not just in launch?
Ease of use, reliable video quality, strong data security, and smooth doctor-patient workflows matter more than just features. If users find it simple and trustworthy, they stick with it.
3. How do telehealth apps handle sensitive patient data securely?
They use encryption, secure cloud storage, and strict access controls. Following regulations like HIPAA or GDPR ensures patient data is handled safely and responsibly.
4. Can a telehealth app integrate with existing hospital systems?
Yes, most modern solutions are built to integrate with EHR/EMR systems, payment gateways, and other healthcare tools through APIs. This helps avoid data silos.
5. What are the biggest mistakes to avoid when building a telehealth solution?
Overloading with features, ignoring user experience, and not planning for compliance early on are common mistakes. Simplicity and clarity always win.
6. How much does it cost to develop a telehealth platform?
Costs vary widely based on features, integrations, and technology. A basic app may start lower, while a scalable, AI-enabled solution can require a larger investment.
7. Who should consider investing in telehealth app development today?
Hospitals, clinics, startups, and even individual practitioners looking to expand reach, improve patient care, or streamline operations can benefit from it.